You will need to wear an eye patch for a short time.įlashing lights and floaters may continue for a while after surgery. Your ophthalmologist will prescribe any necessary medications for you and advise you when to resume normal activity. You can expect some discomfort after surgery. 
Sometimes vitrectomy is combined with a scleral buckle. Your body’s own fluids will gradually replace the gas bubble. The vitreous gel, which is pulling on the retina, is removed from the eye and usually replaced with a gas bubble. Sometimes this procedure can be done in the ophthalmologist’s office. Your ophthalmologist will ask you to maintain a certain head position for several days. The gas bubble pushes the retinal tear closed against the back wall of the eye. In this procedure, a gas bubble is injected into the vitreous space inside the eye. This procedure is performed in an operating room. The ophthalmologist often drains the fluid under the detached retina, allowing the retina to settle back into its normal position against the back wall of the eye. This treatment involves placing a flexible band (scleral buckle) around the eye to counteract the force pulling the retina out of place. In each of the following methods, your ophthalmologist will locate the retinal tears and use laser surgery or cryotherapy to seal the tear. The decision about which type of surgery and anesthesia (local or general) to use depends upon the characteristics of your detachment. There are several ways to fix a retinal detachment. Retinal DetachmentsĪlmost all patients with retinal detachments require surgery to return the retina to its proper position. Treatment usually prevents retinal detachment. These treatments cause little or no discomfort and may be performed in your ophthalmologist’s office. Most retinal tears need to be treated with laser surgery or cryotherapy (freezing), which seals the retina to the back wall of the eye. Only after careful examination can your ophthalmologist tell whether a retinal tear or early retinal detachment is present. Some retinal detachments are found during a routine eye examination. Your ophthalmologist can diagnose retinal detachment during an eye examination in which he or she dilates (enlarges) the pupils of your eyes. These symptoms do not always mean a retinal detachment is present however, you should see your ophthalmologist as soon as possible.a gray curtain moving across your field of vision.a shadow in the periphery of your field of vision.These early symptoms may indicate the presence of a retinal detachment: What are the warning symptoms of Retinal Detachment? weak areas in your retina that can been seen by your ophthalmologist.previous retinal detachment in your other eye.The following conditions increase the chance of having a retinal detachment: Fluid may pass through the retinal tear, lifting the retina off the back of the eye, much as wallpaper can peel off a wall. But sometimes the vitreous pulls hard enough to tear the retina in one or more places. Usually the vitreous separates from the retina without causing problems. As we get older, the vitreous may pull away from its attachment to the retina at the back of the eye. 
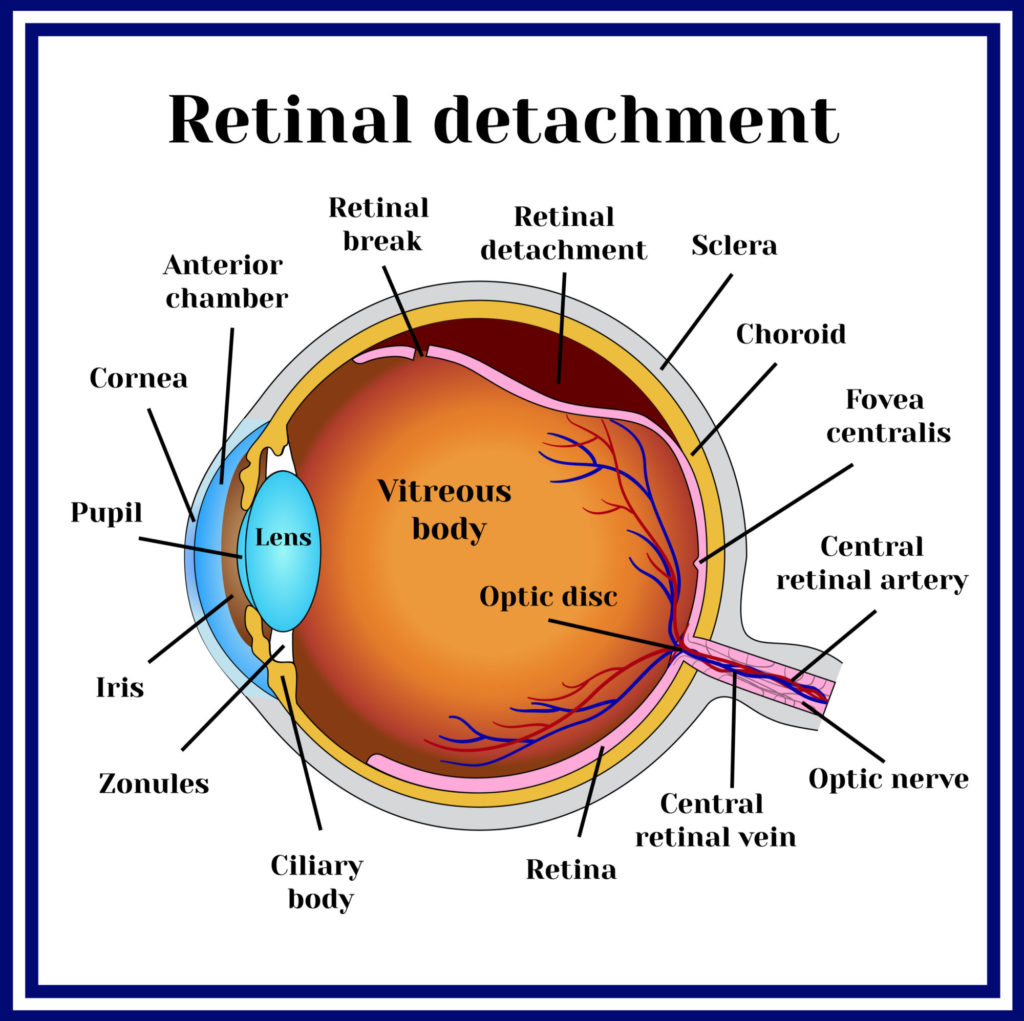
What causes Retinal Detachment?Ī clear gel called vitreous fills the middle of the eye. Vision is blurred, just as a photographic image would be blurry if the film were loose inside the camera.Ī retinal detachment is a very serious problem that almost always causes blindness unless it is treated. The retina does not work when it is detached. You can think of the retina as the film that lines the back of the camera.Ī retinal detachment occurs when the retina is pulled away from its normal position. The lens in the front of the eye focuses light onto the retina. The retina is a nerve layer at the back of your eye that senses light and sends images to your brain. All information taken from the American Academy of Ophthalmology pamphlet on Detached and torn Retina. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
